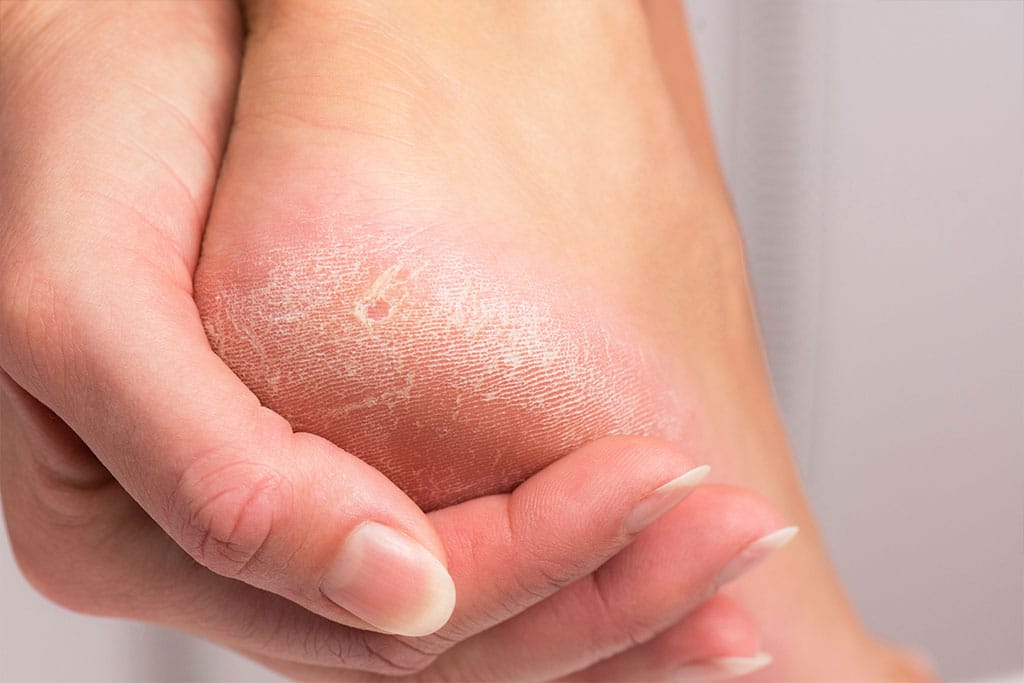
People living with diabetes are more prone to dry and cracked skin. However, neglecting dry skin is not an option in diabetes due to the much higher risk of complications. Moreover, dry skin could be an early sign of diabetes getting worse or a person not controlling blood glucose adequately.
Higher blood glucose may cause dry and cracked skin. It is also worth noticing that fasting blood glucose tests may not always provide the correct information. Generally, A1C is better for understanding how well someone controls blood glucose, as it represents an average of blood glucose level for the last 2 to 3 months.
In diabetes, there is a considerably altered blood supply to the skin. It means a poor flow of oxygen and nutrients. It ultimately leads to dry skin, skin that is prone to various infections.
In diabetes, other protective mechanisms are not working correctly. Autonomic neuropathy means that the body is unable to send signals to the skin as needed. It means that local glands cannot produce moisture, or oil as needed, thus increasing the risk of dry and cracked skin.
Some Tips For Managing Dry Skin in Diabetes
- Avoid harsh soaps. Some soaps have a strong drying effect. One should opt for mild shampoos, soaps, and bathing gels. It is a good idea to opt for products that have added retinoids for extra skincare.
- Keep it hydrated: One should apply mild moisturizers immediately after taking a bath to ensure that no moisture is lost. Further, one may opt for creams or ointments with hydrating and antimicrobial properties. Such creams can be used more frequently. Especially applied on body parts more prone to drying like hands, feet, legs, and so on. It may be a good idea to use cream with moisturizing and antimicrobial properties before going to bed, as it may help prevent infections.
- Soothe, but never scratch: There are many ways of soothing dry and itchy skin. For example, one may take a shower or apply the cream. In addition, an air humidifier may be a way to reduce the risk of dry skin.
- Check skin every day: Sometimes, dryness and cracks may occur in the least expected places. Especially inspect heels and closely examine your toes. Feet are most prone to cracks, infections, difficult to treat wounds. Even worse, they are the first to lose sensation in peripheral neuropathies.
- Treat cracks immediately: Cracks are much worse than dryness. It already means that the skin is broken, and there is a high risk of infection. Thus, moisturizers would not be enough. Instead, one should apply a cream that improves local moisture level along with antiseptic properties.
- Wear loose-fitting clothes: When living with diabetes, protecting feet is essential, but equally vital is taking care of the rest of the body. Thus, wear loosely fitting underwear made of pure cotton and wear loose clothes that allow air to flow through.
Ultimately, if nothing seems to help, do not hesitate to seek medical attention. In diabetes, it is always good to seek medical help earlier than later.